Bidirectional Mendelian Randomization Analysis Reveals Causal Associations Between Autoimmune Diseases and Colorectal Cancer
DOI:
https://doi.org/10.14740/wjon2732Keywords:
Colorectal cancer, Autoimmune diseases, Bidirectional Mendelian randomization, Genome-wide association study, Genetic causality, Celiac disease, Rheumatoid arthritisAbstract
Background: Observational studies have reported associations between autoimmune diseases (AIDs) and colorectal cancer (CRC), but whether these relationships are causal remains unclear.
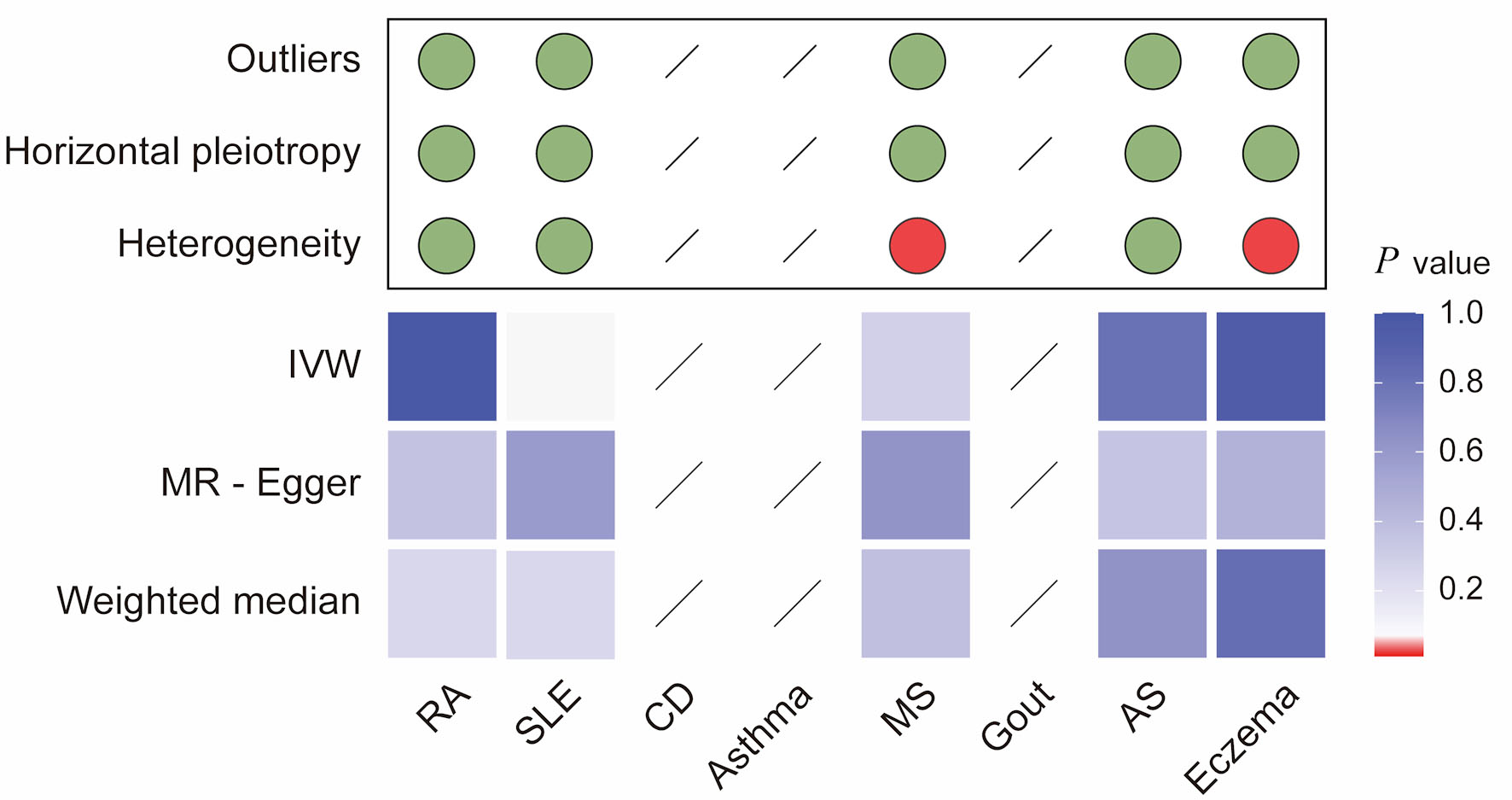
Methods: We performed a bidirectional two-sample Mendelian randomization (MR) analysis to evaluate the causal effects of eight prevalent AIDs—systemic lupus erythematosus (SLE), rheumatoid arthritis (RA), ankylosing spondylitis (AS), gout, multiple sclerosis (MS), celiac disease (CD), eczema, and asthma—on CRC risk, and to examine the possibility of reverse causation. Genome-wide association study (GWAS) summary statistics from individuals of European ancestry were analyzed. The inverse-variance weighted (IVW) approach served as the primary MR estimator, with MR-Egger regression and the weighted median method applied as complementary analyses. Robustness was further evaluated through sensitivity analyses, including assessments of heterogeneity and horizontal pleiotropy.
Results: Genetically predicted CD was associated with a reduced risk of CRC (IVW odds ratio (OR) = 0.94; 95% confidence interval (CI), 0.89–0.99; P = 0.028). Genetically predicted RA was associated with an increased risk of CRC (IVW OR = 1.06; 95% CI, 1.02–1.11; P = 0.004). No significant causal associations were observed for the other AIDs. Reverse MR provided no evidence that genetic liability to CRC causally influenced the risk of these AIDs. Sensitivity analyses supported the stability of the findings.
Conclusions: This bidirectional MR study provides genetic evidence supporting unidirectional, modest causal effects of specific AIDs (CD and RA) on CRC risk. Further studies are warranted to clarify underlying mechanisms, including immune dysregulation, inflammation, and dietary factors, and to determine clinical implications.
Published
Issue
Section
License
Copyright (c) 2026 The authors

This work is licensed under a Creative Commons Attribution 4.0 International License.









