Functional and Survival Outcomes of Partial Versus Radical Nephrectomy in Renal Cell Carcinoma Patients With Pre-Existing Chronic Kidney Disease: A Real-World Study
DOI:
https://doi.org/10.14740/wjon2728Keywords:
Renal cell carcinoma, Partial nephrectomy, Radical nephrectomy, Chronic kidney disease, eGFR, Overall survivalAbstract
Background: Managing renal cell carcinoma (RCC) in patients with pre-existing chronic kidney disease (CKD) or a solitary kidney requires balancing oncologic control with maximal renal functional preservation. This study analyzes long-term renal function, survival, and complications between partial nephrectomy (PN) and radical nephrectomy (RN) in this high-risk Vietnamese cohort.
Methods: We retrospectively reviewed 90 patients with RCC and reduced pre-operative estimated glomerular filtration rate (eGFR, < 60 mL/min/1.73 m2) or a solitary kidney who underwent surgery at Cho Ray Hospital between 2019 and 2024. Outcomes included changes in eGFR, CKD stage progression, overall survival (OS), cancer-free survival (CFS), and dialysis-free survival (DFS).
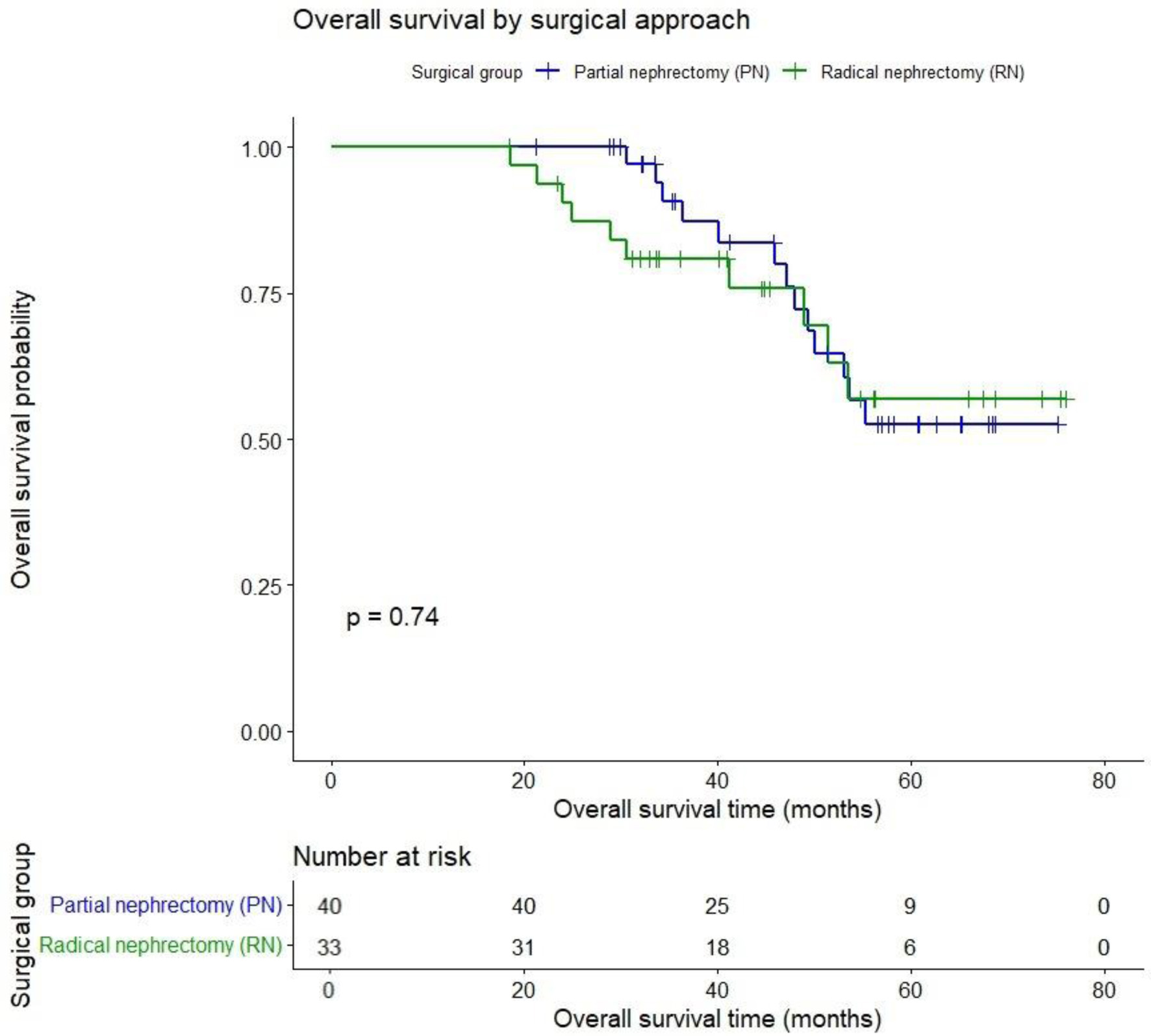
Results: Forty-one patients underwent RN and 49 PN. RN cases had significantly larger tumors and higher RENAL complexity scores (P < 0.001). At a mean follow-up of 45.7 months, PN demonstrated a smaller eGFR decline (−13.2 ± 3.5 mL/min/1.73 m2) compared with RN (−23.3 ± 6.0 mL/min/1.73 m2) (P < 0.001), including in the subgroup with eGFR ≤ 45 mL/min/1.73 m2 (P = 0.002). CKD stage progression occurred in 100% of RN versus 62.2% of PN patients. Long-term OS, CFS, and DFS were comparable between groups (all P > 0.05). Age (hazard ratio (HR) 1.1) and positive proteinuria (HR 5.4) were independent predictors of overall mortality.
Conclusions: PN is the preferred strategy for RCC patients with compromised renal function, when technically feasible, due to its superior functional outcomes. We propose a proteinuria-driven risk stratification approach; the presence of pre-operative proteinuria should strongly favor nephron-sparing surgery and necessitate rigorous long-term nephrological co-management to optimize survival.
Published
Issue
Section
License
Copyright (c) 2026 The authors

This work is licensed under a Creative Commons Attribution 4.0 International License.









