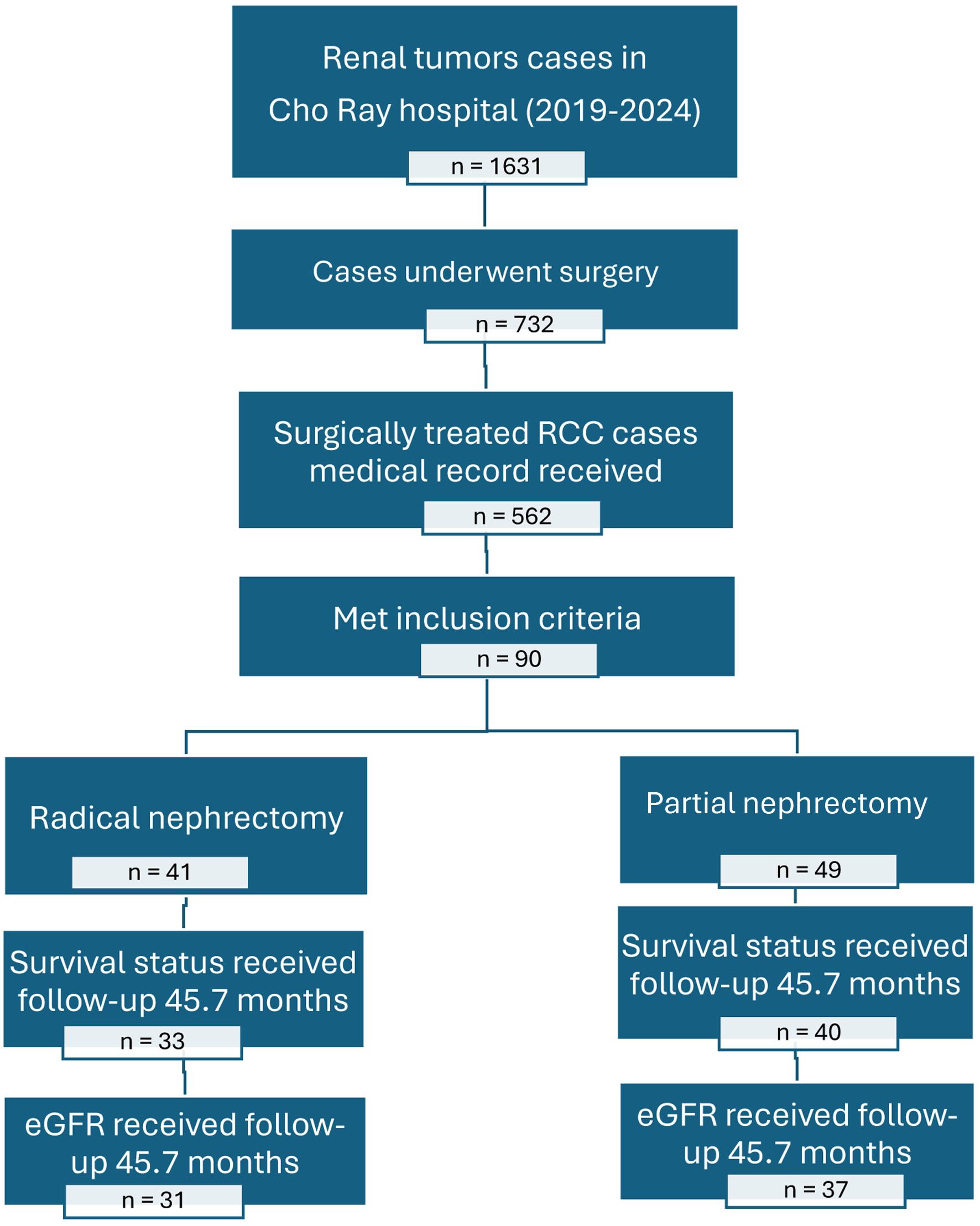
↓ Figure 1. Patient selection and follow-up flow
diagram for renal cancer study at Cho Ray Hospital (2019–2024). Note: Total patients (N = 90): RN
group (n = 41); PN group (n = 49). Excluded from survival analysis (n = 17): loss to follow-up (n = 12);
incomplete oncological records (n = 5). Final survival analysis cohort (N = 73): RN group (n = 33); PN
group (n = 40). Final functional analysis cohort (N = 68): excluded (n = 5) due to missing 12-month
creatinine data.